Recent Posts
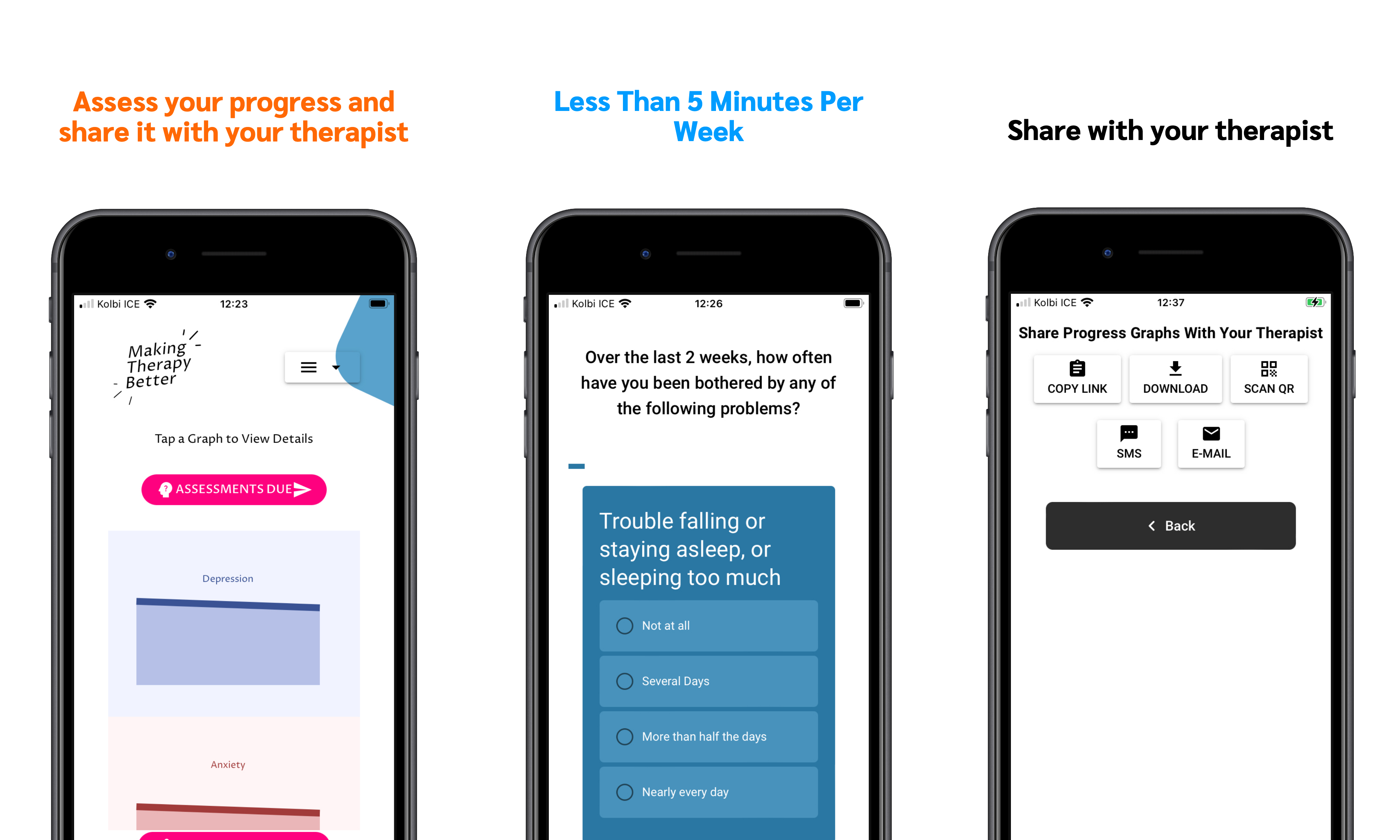
New App Shows What's Working in Psychotherapy
Bruce Wampold, PhD
How to Talk to Your Therapist About Your Progress in Therapy
Bruce Wampold, PhD
Why Using this App can Make Your Therapy Better
Bruce Wampold, PhD
Using Measurement-based Care (MBC) to Make Clinical Decisions
Bruce Wampold, PhD
Talking to Patients as Part of Measurement-Based Care
Bruce Wampold, PhD
Dr. Bruce Wampold on How to Make Therapy Better
Bruce Wampold, PhD
Administering Assessments: The Pragmatics of Measurement-Based Care (MBC)
Bruce Wampold, PhD
What to Measure In Measurement-Based Care
Bruce Wampold, PhD
An Introduction to CarePaths’ Approach to MBC
Bruce Wampold, PhD